I recently took an excellent online tutorial on Breast Implant Associated Anaplastic Large Cell Lymphoma presented by Dr. Mark Clemens of M.D. Anderson Cancer Center. Here is some information from that tutorial as well as information from the American Society of Plastic Surgeons and the American Society for Aesthetic Plastic Surgery. I have also included information from an article in JAMA (Journal of the American Medical Association) Oncology published last week and some of my own take on this really weird disease. Warning: this is a long one.
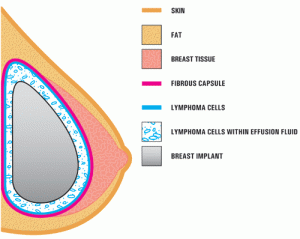
This is a schematic of BIA-ALCL. It is not breast cancer. It is cancer of the breast implant capsule.
Q: What is BIA-ALCL?
A: BIA-ALCL is a rare type of lymphoma that has been found in proximity to breast implants. BIA-ALCL is not a cancer of the breast tissue itself. It is cancer of the breast implant capsule. How weird is that???
Q: What are the symptoms of BIA-ALCL?
A: BIA-ALCL usually develops as a swelling of the breast 2 to 28 years after the insertion of breast implants, which may present as fluid collecting around the implant. It can also present as a lump in the breast or armpit.
Q: What is the risk of developing BIA-ALCL?
A: Early in 2016 the FDA issued a report that it had received 258 adverse event reports of breast implants and ALCL. For a frame of reference, both ASPS and ASAPS data report that approximately 300,000 breast augmentations are performed annually.
A: The lifetime risk for BIA-ALCL in previous epidemiological studies ranges from 1:30,000 to 1:50,000.
A: The figure derived and issued by the Australian government was in the range of 1:1,000 to 1:10,000 for Australian/New Zealand patients with textured/polyurethane implants. Polyurethane implants are not available in the United States.
A. An article published last week (Jan. 4, 2018) in JAMA Oncology and picked up by Newsweek looked at the a large number of women with breast implants in the Netherlands. Almost one half of the implants used in the Netherlands are textured. This is in contrast to the implants used in the United States which are mostly smooth. This study confirmed that this disease occurs with textured breast implant, particularly implants with macrotexturing. The implant specific risk in macrotextured implants like those made by Allergan and Biocell was 1:3817. The risk in microtextured implants like those made Silimed was 1:7788 and by Mentor was 1:60,631. The reasons for that difference is not yet clear but may be related to the increased surface area of the macrotextured implants which could allow for greater bacterial contamination.
A. Risk may also be somewhat influenced by geography (where you live) and genetics (who your parents are). There is increasing evidence that certain bacteria and bacterial biofilm may be causative. Infectious agents are a cause in several other types of tumors such as liver cancer (hepatitis virus) and Burkitt’s Lymphoma (malaria and Epstein Barr Virus). There are also many cancers that tend to run in families such as breast and ovarian cancer, some colon cancers, leukemia, malignant eye tumors to name a few. There may be a genetic susceptibility to BIA-ALCL.
Q: Is there such a thing as ALCL in breasts without implants.
A: Yes but it is very rare. According to the recent JAMA report out of the Netherlands, the risk of ALCL in the absence of implants is 1 in 35,000 at 50 years of age and 1 in 7000 at 70 years of age. The risk in women with implants (all types) is 1 in 7000 at 75 years of age. By contrast, the lifetime risk of breast cancer for women according to the National Cancer Institue is about 1 in 8.
Q: How is BIA-ALCL treated and what is the prognosis?
A: Current recommendations for the treatment of BIA-ALCL call for bilateral capsulectomy and removal of the breast implants. In all but a few cases, the disease has been fully resolved by this surgery alone. The majority of patients require no additional treatment.
Q: Are some patients at greater risk than others?
A: It is not possible to predict who will develop BIA-ALCL, and while the Australian Government reports a higher risk of BIA-ALCL in those patients with textured/polyurethane implants, the data is not yet well established. This risk remains far less than that other known risks, such as capsular contracture.
A: It has occurred in women who have breast implants for both cosmetic and reconstructive purposes.
A: BIA-ALCL has occurred in women with both saline and silicone implants.
Q: Should patients have their implants removed?
A: Neither the FDA nor the Australian Government’s report suggest additional screening or removal of implants for asymptomatic women.
Q: Should women with breast implants be screened for BIA-ALCL?
A: Expert opinion is that asymptomatic women without breast changes do not require more than routine follow-up. If a patient experiences a change in her breasts – especially if there is swelling or a lump – she should undergo examination and appropriate imaging, including ultrasound and fine needle aspiration of any peri-implant fluid.
Q: What causes BIA-ALCL?
A: ASPS, ASERF, the FDA, and the implant manufacturers are working proactively to study BIA-ALCL. To date, no specific causal factors have been identified. Implant texturing, bacteriologic contamination, and genetic factors have been implicated and are undergoing further study.
A: Bacteria have been identified within the lymphoma and around implants in affected breasts, and there is accumulating evidence that a long-term inflammatory response to the presence of these bacteria is one of the factors that may cause BIA-ALCL. Research is ongoing and cases are being monitored through the PROFILE registry.
A: Genetic factors may play a role. The Australia/New Zealand risk appears higher than other studies have indicated. Some geographic areas have reported very few cases. Ongoing data collection worldwide will help to determine whether or not there are any genetic propensities for this disease.
Q: Do ASAPS and ASPS recommend against the use of textured implants?
A: The available data does not support discontinuance of textured implants. The best practice is always for the physician to discuss with each patient the known risks and potential complications associated with any procedure. It is important for the patient and her doctor to frankly discuss all options available, and the risks involved.
A: Every plastic surgeon offers patients options regarding breast implants in terms of sizing, shape, and surface. Textured implants may offer advantages when placed subglandularly (lower risk of capsular contracture), and when an anatomically shaped implant is utilized (lower risk of malrotation). Depending on a particular patient’s needs, a textured implant may be preferable. The plastic surgeon must provide a frank and transparent discussion regarding the benefits and risks of implants, both smooth and textured. The patient must then make an informed decision, based upon her own assessment of her needs and the risks involved.
A: Every plastic surgeon needs to help each individual patient make her own decision about which implant she prefers in a fully transparent manner. This involves weighing any possible increased risks against the advantages offered by a particular type of implant. It is critical that the patient makes a fully informed decision following a full discussion of the risks and benefits.
Q: What does Dr. Sowder think of textured implants?
A: Geeze, I’m glad you asked. I have never been a big fan of textured implants and have used them very infrequently over the years. The main reason for this is that I do not use many anatomic (tear drop shaped) implants which are always textured. I have found these implants, in my hands, to require more revision that smooth, round implants. Also, and I have blogged about this many times, I don’t think anatomic implants make a difference in the vast majority of patients so there is not reason to use them. Anatomic implants are textured so they “stick” and stay put and do not rotate or flip. If a smooth round implant rotates or flips, it does not change the shape of the breast. I consider myself lucky not to have many patients with textured implants out there. I am a worry wart by nature. If my current practice were heavy into textured anatomics, I would be questioning the wisdom of this at least until we know more about BIA-ALCL. There are some plastic surgeons out there who are very evangelical about using anatomic implants (and often times paid con$ultant$ to implant manufacturers) and rather than say, “Whoa Bessie, let’s see how this all unfolds”, some of them are digging in and minimizing the risk of BIA-ALCL which seems to go up with every new study. This sort of stuff makes me cranky. One very difficult issue is that of textured tissue expanders used to stretch out the skin and muscle for implant based breast reconstruction. All of the expanders are anatomic and thus need to be textured so they don’t rotate of flip. I no longer do breast reconstruction but if I did, I would still use textured expanders because there is no alternative.
Q: Have there been any deaths due to BIA-ALCL?
A: There have been 12 confirmed deaths, including 6 in the United States, attributed to BIA-ALCL since the disease was first reported nearly 20 years ago.
Q: What is the recommended clinical response to a patient presenting with symptoms that could be attributable to ALCL?
A: As in all diseases, the first step is to establish a diagnosis. Depending on the extent of the BIA-ALCL, treatment would always involve implant removal and total capsulectomy and, if indicated, chemotherapy. The recent JAMA article reported over 90% of women who underwent proper therapy as having complete remission.
A: In July 2016, ASPS and ASAPS issued a joint “Tear Sheet” describing the recommended clinical protocol for patients presenting with symptoms that could be attributable to BI-ALCL. For a copy of the ASPS/ASAPS Tear Sheet please go to: Joint-ASPS-ASAPS Statement On Breast Implant-Associated ALCL
Access on the ASAPS website at: http://www.surgery.org/professionals
This protocol formed the framework for the international recommendations by the National Comprehensive Cancer Network (NCCN) for the diagnosis of BIA-ALCL and can be accessed at nccn.org.
Q: How is BIA-ALCL diagnosed?
A: If a woman develops swelling in an augmented breast, she should undergo an ultrasound scan. If fluid is detected, it should be drained and tested with CD30 immunohistochemistry to diagnose BIA-ALCL. Mammograms are not useful in diagnosing BIA-ALCL. In confirmed cases MRI and PET/CT scans may be performed to help stage the disease.
Q: How is organized plastic surgery working with the FDA to study BIA-ALCL?
A: The Plastic Surgery Foundation (PSF) created PROFILE (Patient Registry and Outcomes for Breast Implants and Anaplastic Large Cell Lymphoma, Etiology and Epidemiology) in 2012, a collaboration with the FDA. Any suspected or confirmed cases of BIA‐ALCL should be reported for inclusion in the PROFILE registry at ThePSF.org/PROFILE.
A: PROFILE is collecting data both retrospectively and prospectively on confirmed cases of BIA-ALCL.
A: The primary goal of PROFILE is to better understand the role of the breast implants in the etiology of BIA-ALCL. The research hopes to identify potential risk factors, diagnostic predictors, and the best ways to manage this disease. In addition to providing health care practitioners and patients with information about the diagnosis and treatment of ALCL, the confirmed cases will assist with further analytical epidemiological studies.
Q: Where can I find more information on BIA-ALCL?
A: Additional information and resources on BIA-ALCL are available online at www.plasticsurgery.org/alcl and by searching “ALCL” on RADAR.
Reporters seeking information or plastic surgeons contacted by a member of the media are encouraged to forward inquiries to Adam Ross, ASPS integrated communications manager at aross@plasticsurgery.org or 847-228-3361. ASAPS members are encouraged to contact Leigh Hope Fountain, ASAPS director of Public Relations, at leigh@surgery.org or 561-7917




 @lisalynnsowder
@lisalynnsowder
